It only takes a few seconds of watching rugby before you realise why there might be injuries involved. The sheer velocity at which some players travel across the pitch and collide with each other means that problems are inevitable and unavoidable.
Rugby injuries occur more frequently during matches than during training. Due to the frequent physical contact during rugby the incidence of injury is relatively high, with hamstring muscle injuries, ankle sprains, head injuries, shoulder injuries and thumb injuries all common.
The injuries occur most often during collisions such as during tackling, rucking and mauling. Upper limb injuries occur frequently in rugby due to the ball handling and physical contact nature of the sport. Shoulder injuries such as collar bone fractures and Acromioclavicular sprains can lead to a prolonged injury lay off, as can thumb sprains and thumb dislocations.
And it’s for that reason we have decided to arm you with the knowledge you need to prevent and treat, if possible, your rugby injuries.
Starting with the hamstring strain…
Hamstring Strain
What is it?
Full time training in the professional rugby union era has led to players being bigger, fitter, faster and stronger than ever before. These increased physical demands have added extra strain and risk to the lower limbs and with that, and increase in injuries. The hamstring strain is a prime example, being the most common injury to affect England’s World Cup winning squad back in 2003.
During sprinting activities, the hamstring muscle can be forcibly stretched beyond its limits and the muscle tissue becomes torn. A tear in a muscle is referred to as a strain and, depending on its severity, is classified as a first, second or third degree strain.
Prevention
A warm up prior to matches and training is thought to decrease muscle strain injuries because the muscle is more extensible when the tissue temperature has been increased by one or two degrees. A good warm up should last at least 20 minutes, starting gently and finishing at full pace activity. Practicing sport specific activities helps tune coordination and prepare mentally for competition.
We recommend compression shorts for providing extra warmth around the Hamstring region.
Treatment
The immediate treatment of any muscle injury consists of the PRICE protocol – protect, rest, ice and compression and elevation (never apply ice directly to the skin). All injuries should be reviewed by a doctor or chartered physiotherapist. Depending upon the severity of the hamstring injury, the leg must be rested from sporting activity for between a couple of weeks and 3 months.
We recommend the use of an ice bag for the safe application of ice.
Acromio Clavicular Joint Sprain
What is it?
The Acromio Clavicular joint, or the ‘AC’ joint is part of the shoulder complex. Its exact location is situated at the outside point of the collar bone where it attached to the front of the should blade.
A sprain of the AC joint refers to damage to the ligaments of the joint. The AC joint ligaments are most commonly damaged through a fall onto the tip of the shoulder, although as we mentioned earlier, the frequency at which rugby players get injured during tackles means this injury is never too far away.
Prevention
There are ways to reinforce and shore-up the ligaments of the AC joint. Many rugby players find that the reassurance provided by a shoulder support, such as our Ultimate Performance Neoprene Shoulder Support, can be helpful.

However it’s worth taking in to consideration that due to the nature of rugby, where collisions are frequent and hard, it is impossible to totally prevent these injuries.
Treatment
In the initial stage of the injury pain-relieving medication is obviously helpful. Ice packs should be applied to the injured shoulder for 20 minutes every two hours (never apply ice directly to the skin).
A chartered physiotherapist can apply a taping technique, which will push the collar bone downwards, and in more severe AC joint sprains the shoulder may be put in a sling and rested. In more minor AC joint sprains, where there is only a small amount of ligament damage, it may be possible to resume rugby activities in 7-10 days.
Fracture Dislocation of the Thumb
What is it?
This injury has its roots as far back at the 1800’s. Descried by Dr Edward Bennet, who suffered a fracture dislocation of his thumb while horse riding in 1885, it is often known, or referred to as ‘Bennet’s Fracture’.
Anatomically speaking it is a fracture of the joint surface between the thumb, wrist and subsequent detachment of the deep ligaments which normally stabilise the joint.
Due to the long-term problems and functional instability that can occur, many orthopaedic consultants advocate fixing the problem surgically.
Prevention
Not a great deal. Get your chartered physiotherapist to tape your thumb, but even then, a fracture dislocation of the thumb may occur due to the collision nature of rugby.
For some taping options, check out our range of taping and strapping.
Treatment
As far as thumb injuries go, this is a pretty nasty one. It can cause potentially long-term functional impairment of hand function, that’s means all fracture dislocations of the thumb should be assessed by an orthopaedic consultant.
Of course, as is usual with a lot of injuries, in the firs few days following a fracture dislocation of the thumb it is important to follow the PRICE protocol – protection, rest, ice, compression and elevation (never apply ice directly to the skin).
Icing the area for twenty minutes every couple of hours may help allevite the pain but medication subscribed by a doctor may be necessary.
Surgery is often required for this injury and the surgeon may immobilise the thumb in a plaster. Once this is removed, some form of protection for the joint is necessary during the rehab period.
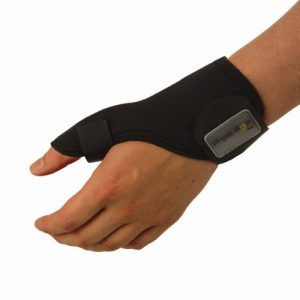
A thumb stabiliser such as the PhysioRoom.com Thumb Stabiliser Support Splint can be helpful in protecting the joint between exercise sessions.
Head Injuries
What are they?
Head injuries range from superficial facial injuries, scalp lacerations and broken noses to severe concussions. Some researchers have reported that they account for over 20% of all rugby union injuries.
Prevention
Rugby headgear is typically a soft helmet that covers the forehead, skull and ears. In Japan these items are compulsory during rugby union. Research has shown that headgear is effective in reducing the incidence of superficial head injuries, such as lacerations.
Treatment
All head injuries should be assessed by a doctor as soon as possible. Lacerations and broken noses can be dealt with by doctors in the emergency department. International Rugby Board (IRB) rules state that “a player who has suffered concussion shall not participate in any match or training session for a minimum period of three weeks from the time of injury, and may then only do so when symptom free and declared fit after a proper medical examination.”

To help tend and protect any cuts or wounds, try the PhysioRoom Mini First Aid Kit!
Sprained Ankle
What is it?
A sprained ankle is one of the most common injuries caused by participation in sports, rugby included. It refers to soft tissue damage (mainly ligaments) around the ankle, usually caused when the ankle is twisted inwards.
As well as damage to the ligaments, the capsule that surrounds the ankle joint can also be damaged. The damage causes bleeding within the tissues, which produces a swollen ankle that can be extremely painful.
Prevention
Taping and bracing the ankle can help to reduce the risk of ankle sprains. Previous research has shown the injury incidence in people with taped ankles was 4.9 ankle sprains per 1000 participant games, compared with 2.6 ankle sprains per 1000 participant games in students wearing ankle braces. This compared with 32.8 ankle sprains per 1000 participant games in subjects that had no taping or bracing.
Treatment
In the first few days following an ankle sprain it is important to follow the RICE protocol – rest, ice, compression and elevation (never apply ice directly to the skin). Ice packs for a period of twenty minutes every couple of hours may help with the pain but pain-relieving medication may also be necessary. It is important not to put too much weight on the damaged ankle, so walking should be avoided if it is painful.
For some extra ankle support, check out the AirCast a60 Ankle Brace.




