What is a High Ankle Sprain?
A sprained ankle is one of the most common injuries caused by participation in sports. It refers to soft tissue damage (mainly ligaments ) around the ankle joint. A high ankle sprain refers to ligament damage at the joint between the shin bone (tibia) and splint bone (fibula). This joint is referred to as the ankle syndesmosis.
A syndesmosis is a joint where the two bones are bound tightly together by ligament tissue. The ankle syndesmosis refers to the fibrous band of ligament tissue which connects the shin bone and fibula. Specifically, this refers to the ‘interosseous membrane’ between the two bones, as well as the anterior (front) and posterior (back) tibio-fibular ligaments.
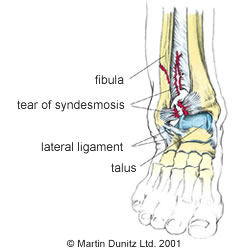
In the case of a high ankle sprain, the mechanism of injury is excessive ankle dorsi-flexion (where the toes come up towards the knee) as well as external rotation of the shin, which causes damage at the ankle ‘syndesmosis’.
As well as damage to the ligaments, the capsule that surrounds the ankle joint can also be damaged. The damage causes bleeding within the tissues but, unlike a medial or lateral ankle sprain, the ankle joint doesn’t usually swell too much.
Syndesmotic ankle sprains can be classified as follows:
- First degree, where only a few ligament fibres are damaged within the interosseous membrane
- Second degree sprain refers to more extensive damage to the interosseous membrane with some widening of the tibio-fibula joint
- Third degree sprain refers to a complete rupture of the interosseous ligament with gross widening of the tibio-fibula joint and possible joint dislocation
In the more severe injuries there may be associated bone injury and it is wise to get an x-ray to determine whether there is a fracture.
Signs & Symptoms of a High Ankle Sprain
With a first degree sprain there is usually pain on ankle movement and when the damaged area is touched. Typically, with a second degree sprain the pain is more severe, there may be swelling all around the area and it is painful to walk. With a third degree sprain the pain is excruciating and walking is impossible. A swollen ankle is typical and there may be a visible deformity if the ankle is dislocated. A physiotherapist will differentiate a high ankle sprain from an inversion sprain or other injury.
Treatment for a High Ankle Sprain
What you can do
- Consult a sports injury expert
- Apply ice packs/cold therapy to reduce swelling
- Wear a removable plastic cast for protection
- Wear an ankle support for protection
In the case of a grade three ankle syndesmosis injury then surgery may be required to fix the tibia and fibula back in place. Grade one and two injuries take between one and two months to recover from completely.
In the first 48-72 hours following the injury it is important the follow the PRICE protocol protection, rest, ice, compression and elevation (never apply ice directly to the skin). Ice packs for a period of twenty minutes every couple of hours may help with the pain but pain-relieving medication may also be necessary. The Aircast ankle cryo cuff is the most effective method of providing ice therapy, whilst protecting the injured tissues from further damage, and is the professional’s choice. It can provide continuous ice cold water and compression for 6 hours and significantly reduce pain and swelling.
It is important not to put too much weight on the damaged ankle. Excessive walking should be avoided if it is painful. Ankle injuries can be protected using a plastic cast walker and these are regularly used by Premier League football players.
Where a fracture is suspected an x-ray should be carried out at an accident and emergency department as soon as possible. If a fracture is found or a grade three sprain is diagnosed, the advice of the attending doctor should be followed. It should be borne in mind that some hairline fractures do not show up on x-ray until about 10-14 days after the injury, so if the pain persists medical attention should be sought.
In the case of a grade two sprain, crutches should be used to protect the injured ankle. However, it is important not to be on the crutches for longer than necessary and as soon as the pain allows the patient should begin to gently put weight through the ankle by walking. Plastic cast walker can be very helpful as they allow the patient to walk, protect the injured area and help to resolve ankle swelling.
Once the patient is able walk on the ankle, more active rehabilitation can be started. Manual therapy is then very effective at restoring ankle movement and resolving stiffness. Physiotherapists can help by manipulating and massaging the joint to help restore a full range of movement.
How to Prevent a High Ankle Sprain
What you can do
- Wear an ankle support for protection
- Use a wobble board for ankle strengthening
Ankle instability is characterised by ankle weakness and giving way, even though the ankle ligaments are intact and the joint is mechanically stable. It is due to an impairment of proprioception, which leads to a lack of balance and ankle joint position sense. Proprioception is the mechanism by which nerve receptors in skin, muscle, ligament and joint tissue relay information to the brain about body position sense, where this information is quickly processed and movement strategies are formulated and executed using nerve signals to muscles. This mechanism can help you ‘catch yourself’ when you are about to turn your ankle.
In the unstable ankle these receptors may have been damaged directly during an ankle sprain. This impaired proprioceptive ability may, therefore, lead to a delay in protective muscle activity and the resultant loss of postural awareness and stability around a joint. This may explain why recurrent ankle sprains are so common. Proprioception should be a primary focus of rehabilitation to reduce the risk of re-injury and help ensure a successful return to sport and activity.
A wobble board together with ankle braces are commonly used in the rehabilitation of ankle instability. Wobble boards are designed to assist the re-education of the proprioceptive system by improving sensory receptor function. Previous research has also shown that wobble board training improves single leg stance ability and balance; while other studies have suggested that patients with ankle instability who underwent wobble board training experienced significantly fewer recurrent sprains during a follow-up period than those who did not follow the training programme.
Exercise bands (resistance bands) may also be used to start to encourage range of movement and gentle strengthening exercises. Different levels of resistance can be used so light bands are used at first then as pain, swelling and function all improve the level of resistance can be increased.
Taping and bracing the ankle can also help to reduce recurrent ankle injury. Previous research has shown the injury incidence in students with taped ankles was 4.9 ankle sprains per 1000 participant games, compared with 2.6 ankle sprains per 1000 participant games in students wearing ankle braces. This compared with 32.8 ankle sprains per 1000 participant games in subjects that had no taping or bracing.
What is a Metatarsal Fracture?
Metatarsal fractures are the most common traumatic foot injuries. Broken metatarsals have been prominent across all professional sports in the past five years, with several high profile athletes suffering metatarsal fractures. Professional football (soccer) players David Beckham, Wayne Rooney, Ashley Cole and Steve Gerrard have all sustained this foot injury in recent years. To understand the metatarsal fractures further it is probably best to start by explaining the anatomy of the foot.
There are five metatarsal bones in each foot. They are the relatively long bones which are located between the ‘tarsal’ bones of the hind-foot and the ‘phalanges’ bones in the toes. Functionally, the ankle and foot have two principle functions: propulsion and support. The metatarsal bones play a major role in these functions. For propulsion they act like a rigid lever and for support they act like a flexible structure that aids balance, thus holding up the entire body.
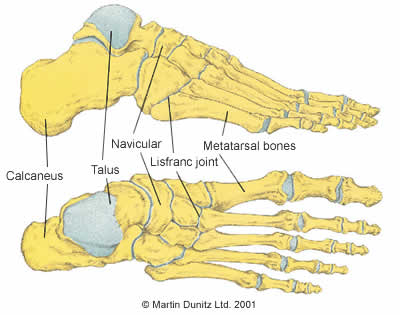
Fractures to the metatarsal bones can be caused by direct trauma, excessive rotational forces or overuse. During football, direct trauma is usually caused by a player accidentally kicking the sole of an opponent’s boot, or by an opponent stepping on a player’s foot. As there is very little soft tissue to protect the top of the foot, bone injuries are common. The second, third and fourth metatarsals are the most commonly fractured with this mechanism of injury, although the fifth metatarsal is fractured more often in soccer.
In repetitive sports like running the metatarsal bones may become overloaded and can become fractured by the stress of impact and possibly by faulty foot mechanics that cause, often the 5th metatarsal to be injured in what is known as a stress fracture. In cycling, the pressure of cleats on the pedals can also lead to irritation and eventual fracture in a similar fashion.
The fifth metatarsal is divided into four anatomic segments (the base, the junction of the base and the shaft, the shaft, and the neck) and different types of fracture can occur at each segment.
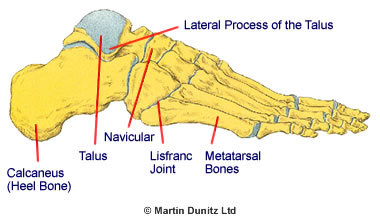
Fractures of the base of the fifth metatarsal are the most common fifth metatarsal injuries, and occur as a result of a twisting injury of the foot or ankle. The ankle rolls inward and there is a strong ligament that attaches to the base of the metatarsal which pulls off a small bone fragment. This type of fracture is invariably treated without surgery, and immediate walking in a removable plastic cast is ideal.
The junction between the base of the metatarsal and the shaft is the area which creates most problems when fractured. The reason for the difficulty is that bone healing relies upon a good circulation, and this particular area of the bone has a notoriously poor blood supply. Fractures of the shaft of the metatarsal occur commonly as a result of twisting of the foot when landing from a jump, for example in ballet dancers, and these heal very rapidly with immobilisation, without any need for surgery. Landing on a hard rock or branch whilst running can also cause similar impact and injury.
Overuse can cause stress fractures of the metatarsals. These fractures are common in army recruits as well as sporting individuals and are commonly known as ‘march’ or stress fractures. The patient will normally report about two weeks of gradually increasing pain in the region before an incident ‘converts’ the stress fracture to a full fracture. The second metatarsal is the most commonly affected, but the fifth metatarsal can also be affected. While the stress fracture of the second metatarsal usually heals well, the healing of a stress fracture to the fifth metatarsal can be more problematic. If a stress fracture is caught early before it becomes a full fracture it is commonly known as a Stress response, as the excess inflammation has not yet led to a fracture and therefore holds a better prognosis. A physiotherapist can help assess gait and identify why this area of the foot may be prone to excessive load. Corrective exercises and strengthening can then be prescribed to prevent further irritation.
Metatarsal Fracture Signs & Symptoms
There is severe and often precise foot pain with a metatarsal fracture and the patient will usually find it difficult to walk. Often there will be pain if the fracture site is touched. A swollen foot is fairly common and bruising may be evident after a day or two.
Treatment for a Metatarsal Fracture
- Consult a sports injury expert
- Apply ice packs/cold therapy to reduce swelling
- Protect the foot with a removable plastic cast
- Use a buoyancy aid for pool exercises
- Use a bone healing system to speed up broken bone healing
If a metatarsal fracture is suspected the patient should be transferred to an emergency department where a doctor can confirm the diagnosis by ordering an x-ray . Immediately following a metatarsal fracture ice therapy can be effective to help with pain relief, although medication prescribed by a doctor is usually necessary. Ice packs for a period of twenty minutes every couple of hours may help with the pain. The Aircast ankle & foot cryotherapy cuff is the most effective method of providing ice therapy. It can provide continuous ice cold water and compression for 6 hours and significantly reduces foot pain and swelling.
The ultimate treatment of Metatarsal fractures varies depending on the type and location of the fracture. If the fracture is due to direct trauma and the fracture fragments are well aligned then the treatment is immobilisation in a removable plastic cast and non-weight bearing for 6 – 8 weeks.
The removable plastic cast is better than a plaster cast, because the boot can be removed for physiotherapy treatment, which is aimed at preventing stiffness in the ankle joint. In addition, cardiovascular fitness can be maintained by performing non-weight bearing exercises in a swimming pool using hydrotherapy aids such as a buoyancy belt.
A removable plastic cast is also usually adequate for ‘march’ (stress) fractures of the second metatarsal and rotational fractures of the fifth metatarsal. However, stress fractures of the base of the fifth metatarsal sometimes show a poor healing capacity. For this reason, many orthopaedic consultants now favour surgical fixation. A small incision is made on the outside border of the foot and a small screw is placed down the middle of the fractured bone. With this method a return to sporting activity is usually possible after 6 – 8 weeks.
Metatarsal Fracture Prevention
If the force applied to the foot during a traumatic incident is high then there is very little that can be done to prevent a metatarsal fracture. However it is always important to wear appropriate footwear that gives the foot some protection and make sure you replace shoes regularly especially for activities such as running or hiking. Running shoes roughly last 500 miles so make sure you monitor this and change them to prevent inadequate shock absorption. If taking on barefoot running this needs to be a slow introduction to avoid injury.
If the injury is a stress fracture then training levels need to be reviewed as well as looking into bone density and diet.

