What is a Torn Cartilage?
A torn cartilage is a common knee injury in sports. The term cartilage tear is slightly misleading, since it is the meniscus within the knee that is actually damaged.
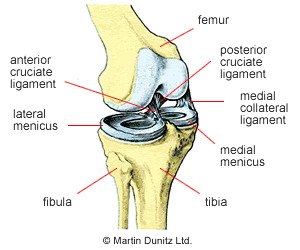
There are two menisci within each knee joint that are made from tough fibrocartilage – hence the use of the term cartilage for this injury. The menisci are roughly semicircular in shape and are markedly thicker around the rim. They are located on the tibial plateau (the top surface of the shin bone) between the shin bone and the thigh bone. The function of the menisci is to increase the congruence and stability of the knee joint and to act as shock absorbers during weight-bearing activity.
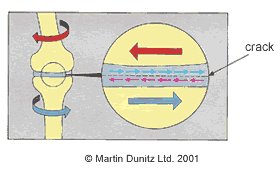
As the knee joint bends the thigh bone usually rolls, spins and glides on the top surface of the shin bone. However, if there is rotation caused by a twist whilst the joint is bearing weight, the menisci can get jammed and nipped in between the two bones. If the force is sufficient, a tear of the meniscus will occur. Sometimes a torn section of meniscus can cause a flap and also get nipped when the joint moves.
Signs & Symptoms of a Meniscus Tear
The Meniscus itself does not have a nerve supply, so no pain emanates from this structure. However, due to the force of the twist there is often associated damage to other knee structures. The most common structures to be damaged are the Medial Collateral Ligament (MCL) and the coronary ligaments, which help attach the menisci to the top of the shin bone. The damage to the joint may cause the knee joint to swell up.
In addition to the lack of nerve supply, the menisci also have a poor blood supply, which means that, depending on the section of meniscus that is torn, the tear is unlikely to heal. As a consequence, the tear produces a flap that interferes with normal joint mechanics. This produces a characteristic ‘clunk’ within the knee when it is bent and straightened and it may cause the joint to lock in one position. Frequently the knee gives way, particularly when walking downstairs.
Torn Cartilage Treatment
In some cases, after the initial knee pain and swelling, the knee joint settles down and normal activities can be resumed. This is because the tear in the meniscus is small or the flap does not affect the joint mechanics. However, in the case of a sporting individual, the flap can cause the knee to sporadically lock or give way, then surgery is required. This is carried out arthroscopically, whereby a small camera and burring device are used by the knee surgeon to remove the flap and smooth off the surface of the meniscus. The patient is usually in hospital for one night and can then begin rehabilitation.
The initial goals of physiotherapy treatment are to reduce knee pain and knee swelling. Ice packs can be applied for periods of twenty minutes every couple of hours (never apply ice directly to the skin as it can cause an ice burn) to relieve pain and reduce bleeding within the tissue. A cryotherapy cuff is the most effective method of providing ice therapy and can be used for the home treatment of knee injuries and knee pain. It can provide continuous ice cold water and compression for 6 hours to significantly reduce knee pain and knee swelling.
A knee brace can restore a degree of knee joint stability, whilst you rebuild the strength around the joint, preventing the feeling that the knee is going to ‘give way’. Together with physiotherapy treatment, a knee brace can help to restore knee joint confidence. Braces can provide stability without compromising knee movement, so can be used during rehabilitation and on return to sporting activities.
Once the surgical wounds have fully healed then hydrotherapy is an ideal method of maintaining fitness. A buoyancy aid can be worn and allows the user to jog in water without touching the bottom of the pool. This helps to restore knee range of movement, as well as providing excellent cardiovascular training and functional rehabilitation of the entire lower limb. It is ideal following cartilage surgery as pool running puts no weight bearing stress on the knee joint and the hydrostatic pressure of the water can help further reduce swelling around the area.
Meniscus Tear Injury Rehabilitation
Stage 1: First 10 days
The following programme is that typically used by a professional football player who has undergone an arthroscopic meniscectomy.
If the medial meniscus (inner side compartment of the knee) has been operated on, the rehabilitation time is usually quicker than if the lateral meniscus (outer side compartment of the knee joint) has been operated on. In the case of an arthroscopic meniscal procedure involving the lateral meniscus the rehab will usually take 6 -8 weeks. In the case of the medial compartment it may be possible to return to sport after 3 or 4 weeks.
Ex-Rangers and Scotland player Ally McCoist once famously returned to playing in less than two weeks after arthroscopic meniscal surgery. The length of rehabilitation is dependent upon which meniscus is affected, exactly where the tear is, the size of the tear and the amount of meniscus which is removed by the surgeon.
On discharge from hospital the patient may be on crutches. With the permission of the consultant, the physiotherapist can begin teaching a normal gait pattern so that the patient can resume walking normally. If there is still a limp it is too early to walk without crutches.
Any residual swelling should be controlled with a compression device such as a cryocuff or flowtron pneumatic unit. These both have the effect of squeezing the knee joint, helping the excess fluid within the joint to disperse.
Isometric quadriceps and hamstring exercises should be initiated:
An isometric quads contraction is achieved by sitting on the floor with the legs straight and then pushing the back of the knee down towards the floor. This contraction should be held for 4 seconds and then relaxed.
To do an isometric hamstring contraction the patient should sit in a chair with the heel to the floor, and then dig the heel into the floor, as if trying to drag the foot backwards. Again this contraction should be held for 4 seconds.
The isometric quads and hamstring work should be done in 5 sets of 10, repeated 3-4 times per day.
Range-of-movement exercises should be initiated as soon as possible. Extension of the knee is achieved via the isometric quads exercises. Knee flexion is regained by sitting on the floor with the knees out straight, and then attempting to bend the knee. This can be made easier by placing something that slides easily, like a plastic bag, under the heel, then sliding the heel up and down. Another method of increasing the knees’ range of movement is to sit in a high chair with the feet hanging free. The affected leg should be swung backwards and forwards, with the range of movement gradually increased over time.
Stage 2: Days 5 to 14
As early as the patient can comfortably bear weight through the affected knee, proprioceptive exercises should be initiated. These improve the stimuli within the body relating to position and movement.
Wobble board exercises to improve proprioception. The patient should balance on the affected leg for 1 minute, then rest. This can be repeated several times.

Proprioceptive exercises using a gym ball. The patient should balance on the affected leg for 1 minute, then rest. This can be repeated several times.

More advanced proprioceptive exercises using the swiss ball. The patient balances on the affected foot with their weight against the gymnastic ball. This can be done with the knee joint at various angles, from straight to bent, according to what the patient can stand. Whilst in these positions the therapist throws the ball and the patient has to balance. 3 sets of 20 catches are normally done, with a rest in between each set.

Range of knee motion can be increased through cycling and wall sliding exercises.
Wall sliding exercises to increase knee range of motion involve sliding the foot up and down as shown. The patient will normally be instructed to perform 5 sets of 20 repetitions.


Once the portals from the arthrosopic surgery have healed and the surgeon has given the go-ahead, exercises in water can begin. These have the advantage of improving and maintaining knee joint range of motion and also strengthening the joint without putting weight through the joint.
Pool exercises are excellent once the surgeon indicates the wounds have healed sufficiently.
Stage 3: Weeks 2 to 6
All the exercises of the previous two phases can be continued. Once the surgeon has given the go-ahead more intense weight-bearing and running can be initiated.
Plyometric exercises using a box, involving landing and taking off in quick succession. Start off slowly and then build the speed at which the exercises are done. The number of repetitions and sets should be gradually progressed.


Jogging should be progressive:
DAY 1: Jog 100 metres, walk 50 metres, with 6 repetitions. Progress to next day activity if there is no swelling or pain.
DAY 2: Jog 150 metres, walk 50 metres, with 6 repetitions. Progress to next day activity if there is no swelling or pain.
DAY 3: Jog 200 metres, walk 50 metres, with 8 repetitions. Progress to next day activity if there is no swelling or pain.
DAY 4: Jog 200 metres, walk 50 metres, with 12 repetitions. Progress to next day activity if there is no swelling or pain.
DAY 5: Jog 2000 metres.
Stage 4: Functional Rehab
The progression to functional activities can begin once the patient can jog without pain and is comfortable doing plyometric drills. The idea of this stage is to progress from gentle exercise to the high intensity at which games are played. All exercises are preceded by a warm up.
Since each exercise is a progression, they should be completed at least one day apart.
Exercise 1
Variable pace running with the gradual introduction of turns.
This involves running round a 20m diameter figure-of-eight course. The figure-of-eight course puts very gentle stress on the knee and prepares the player for later turning drills. The pace is limited to walk, jog or half pace running and is determined by the physiotherapist who shouts out the desired pace. The physiotherapist also shouts the commands stop and start. This re- introduces the player to the variable demands of a game of football.
The session should last about 25 minutes.
Exercise 2
Variable pace running with gradual turns and various starting positions.
The player starts at one end of the course and makes a 30m run up to a 20m diameter semicircle, around which they gently turn before completing another straight 30m run back to the finish. The pace of the run is dictated by the physiotherapist and is either a jog or half pace. The starting position should be different for each run (standing, lying on back, lying on front, sprint start position, squatting, right side lying, left side lying, jumping, hopping, facing backwards).
The player should complete 20 runs.
Exercise 3
A progression of exercise 1.
Variable pace running with slightly tighter turns. The player runs round a 10m diameter figure-of-eight course. The figure-of-eight course puts stress on the knee and prepares the player for later turning drills. The paces used are walking, jogging, half pace running, or three-quarter pace running and is determined by the physiotherapist who shouts out the desired pace. The physiotherapist also shouts the commands stop and start. This re-introduces the player to the variable demands of a game of football.
The session should last about 25 minutes.
Exercise 4
Variable pace running with gradual turns and various starting positions. The player starts at one end of the course and makes a 30m run up to a 20m diameter semicircle, around which they gently turn before completing another straight 30m run back to the finish. The pace of the run is dictated by the physiotherapist and is either three-quarter or full pace. The starting position should be different for each run (standing, lying on back, lying on front, sprint start position, squatting, right side lying, left side lying, jumping, hopping, facing backwards).
The player should complete 20 runs.
Exercise 5
Two 5m diameter circles are placed 30m apart. Traveling at full pace the player makes a run, with a football at the feet, goes around the far circle and then back to the finish.
This should be repeated x 20.
Exercise 6
As Exercise 5, but single cones are used instead of 5m diameter circles.
Exercise 7
Six cones are placed 5m apart in a straight line. The player completes a shuttle run at full pace, turning alternately to the left and right.
This should be repeated x 10.
Before a gradual return to full training the player should be happy with all normal ball work drills, all types of passing (instep, side foot, front foot, outside of foot, side foot volley, laces volley, half volley) over all distances, heading, jumping and heading, and tackling.
Torn Cartilage Prevention
Unfortunately, a torn cartilage is very difficult to prevent. Maintaining quadriceps and hamstring muscle strength, to protect the knee joint, is probably the most effective prevention strategy. As the knee lies anatomically between the ankle and the hip, working on improving balance and ankle strength, such as with a wobble board, as well as glute exercises can help strengthen the whole chain and lessen the load on the knee.