Gilmore’s Groin is a fairly common injury in kicking sports such as football and rugby. This condition is named after Jerry Gilmore, the London surgeon who first recognised this syndrome in 1980. The condition is also known as a sports hernia, but Gilmore’s Groin is a more apt title because, strictly speaking, there is no true herniation.
Gilmore’s Groin is characterised by damage to the tissue that surrounds the Inguinal canal. Specifically, there is a tear to the aponeurosis (a sheet like tendon) of the external oblique muscle and/or a tear to the tendon of the Internal oblique muscle.
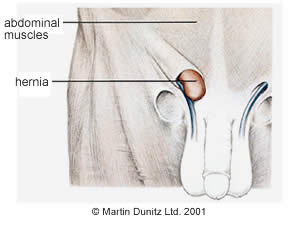
Gilmore’s Groin Signs & Symptoms
The symptoms of Gilmore’s Groin are characterised by pain during sports movements, particularly twisting and turning. This pain usually radiates to the adductor muscle region and even the testicles, although it is often difficult for the patient to pinpoint.
Following sporting activity the person with Gilmore’s Groin will be stiff and sore. The day after sports activity, getting out of bed or a car will be difficult. Any exertion that increases intra-abdominal pressure, such as coughing, sneezing or sporting activity can cause pain. In the early stages, the person may be able to continue playing their sport, but the problem usually gets progressively worse.
Pain in the groin and pelvis can be referred from a number of problems, including injuries to the lumbar spine, the hip joint, the sacroiliac joint, the abdomen and the genitourinary system, so diagnosis of Gilmore’s Groin requires skilful differentiation.
The diagnosis of Gilmore’s Groin is based on the patient’s history and clinical signs. The most notable clinical sign is widening of the superficial Inguinal ring on the affected side, which can be palpated during the physical examination when the scrotum is inverted with the doctor’s finger. Typically, there is specific pain on coughing and sneezing, as well as sitting up and squeezing the legs together.
Gilmore’s Groin Treatment
Conservative treatment with a Chartered Physiotherapist involves stabilising and strengthening the muscles of the core and pelvic region but this is a stop gap at best. In most cases it is usually possible to continue playing sports while wearing compression shorts, until an opportune time can be arranged for surgery. Core strength and stability exercises can be helpful and allow the person to continue competing for a little while longer. However, there usually comes a time when the person can no longer continue because sports performance becomes so impaired. A surgical approach is required to cure the problem.
Successful surgery is dependent upon accurate diagnosis, meticulous repair and adherence to a standard rehabilitation program. Between 1980 and 2000, of 4,500 patients referred to Jerry Gilmore’s clinic in London, 2,700 were treated surgically. Of the professional soccer players treated surgically, Gilmore reported a success rate of 97%.
A specific rehab program must be carefully adhered to. This prohibits sudden twisting and turning movements, with a gradual progression of pelvic muscle stability, flexibility and strength. Upright standing and walking is encouraged from day one. Straight line jogging can be initiated between 10 and 14 days post-op and straight line sprinting is usually started after 3 weeks. Thereafter, sports specific rehabilitation is graduated, with a return to competition usually possible after five weeks.
The Gilmore protocol warns that some stiffness and discomfort may occur the day after sporting activity and advocates some activity 7 days a week to remedy this.
Gilmore’s Groin Rehabilitation
The following is an example rehabilitation program for a professional footballer who has undergone surgical repair of a torn conjoined tendon and oblique aponeurosis’ ‘Gilmore’s Groin’.
The principle behind the exercises is that if certain specific muscles can be recruited or contracted, the trunk and pelvis will have much better support. This helps to counteract the shearing forces during sport, which can lead to overuse conditions such as Gilmore’s Groin.
Post-op: Day 1
- Check wound and start a daily change of dressing. The patient should be independently mobilising into an upright position, in order to promote scarring in functional position.
- Discharge from hospital at discretion of surgeon.
Isometric abdominal exercises: Lie back with knees bent. Slide hands up thighs, then hold for four seconds at half way position (6 repetitions).
Knee rolls: In the same position as above, roll both knees to the left, then to the right (6 repetitions).
Lying on back: Bend left knee up to chest and straighten right knee out and keep it raised 10cm off the bed. Repeat other side (6 repetitions).
Post-op: Days 2-5
- Carry out daily exercises as for day one (8 repetitions), three times each day.
- Initiate gentle cardiovascular work in straight lines (bike, stepper, cross trainer, etc).
Post-op: From Day 6
- Continue exercises as for days 2-5 (10 repetitions), three times each day.
- Continue cardiovascular work in straight lines (bike, stepper, cross trainer, etc).
- Initiate Core Strength exercises – 2 sets of 6 exercises.
Core Strength Exercises
Side holds with leg lift: Lay on your side, with your trunk straight, resting on the elbow. Raise the upper leg and hold for four seconds, then relax.
Trunk twists (med ball between knees): Balance on the swiss ball, with a medicine ball held between the knees. Hold a medicine ball in outstretched arms and twist slowly from from left to right, then back again.
Lunges (use med ball and twist): Lunge forward. Progress to lunging forward with a medicine ball in outstretched arms and then twist in alternate directions, right then left.
Ball rolls: Have your arms on the floor and feet balancing on the medicine ball. Roll first to the left then to the right.
Adductor strength: Lying on the side, raise the ‘lower’ leg up and hold for four seconds. Repeat for the other side.
Post-op: From day 7
- Discontinue ‘bed’ exercises.
- Progress core strength exercises to 2 x 8 repetitions.
- Continue bike, stepper, cross trainer progression.
- Once the wound is closed and stitches removed initiate hydrotherapy rehab – aqua jogging in straight lines wearing buoyancy belt.
Post-op: From day 9
- Progress core strength exercises to 2 x 10 repetitions.
- Continue bike, stepper, cross trainer progression.
- Continue hydrotherapy progression.
Post-op: From day 12
- Progress core strength exercises to 3 x 8 repetitions.
- Continue bike, stepper, cross trainer progression.
- Continue hydrotherapy progression.
Post-op: From day 15
- Progress core strength exercises to 3 x 10 repetitions.
- Continue bike, stepper, cross trainer progression.
- Initiate straight line jogging (treadmill) at slow speed.
- Continue hydrotherapy progression.
Post-op: From day 18
- Progress core strength exercises to 3 x 12 repetitions.
- Continue bike, stepper, cross trainer progression.
- Progress speed of straight line running (treadmill).
- Continue hydrotherapy progression.
- Initiate single plane power exercises – squats, calf raises, clean and jerk.
Post-op: From day 21
- Progress core strength exercises to 4 x 10 repetitions.
- Continue bike, stepper, cross trainer progression.
- Progress speed of straight line running to 3/4 pace (treadmill).
- Continue hydrotherapy progression.
- Continue progression of single plane power exercises – squats, calf raises, clean and jerk.
Post-op: From day 24
- Progress core strength exercises to 4 x 10 repetitions.
- Continue bike, stepper, cross trainer progression.
- Progress speed straight line running to sprints. Introduce ball work to 75% straight runs.
- Continue hydrotherapy progression.
- Continue progression of single plane power exercises – squats, calf raises, clean and jerk.
- Initiate functional running patterns
Functional Running Pattern Exercises
Exercise 1
Variable pace running with the gradual introduction of turns.
The player runs round a 20m diameter figure-of-eight course. The figure-of-eight course puts very gentle stress on the knee and prepares the player for later turning drills.The pace is limited to walking, jogging or half pace running and is determined by the physiotherapist who shouts out the desired pace. The physiotherapist also shouts the commands to stop and start. This re-introduces the player to the variable demands of a game of football.
The session should last about 25 minutes.
Exercise 2
Variable pace running with gradual turns and various starting positions.
The player starts at one end of the course, makes a straight 30m run up to the 20m diameter semi-circle, around which he gently turns before completing another straight 30m run back to the finish. The pace of the run is dictated by the physiotherapist and is either a jog or half pace. The starting position should be different for each run (standing, lying on back, lying on front, sprint start position, squatting, right side lying, left side lying, jumping, hopping, facing backwards).
The player should complete 20 runs.
Exercise 3
Variable pace running with slightly tighter turns. The player runs round a 10m diameter figure-of-eight course. The figure-of-eight course puts stress on the knee and prepares the player for later turning drills.The paces used are walking, jogging, half pace running, and three quarter pace running and are determined by the physiotherapist who shouts out the desired pace. The physiotherapist also shouts the commands to stop and start. This re-introduces the player with the variable demands of a game of football.
The session should last about 25 minutes.
Post-op: From day 28
- Progress core strength exercises to 4 x 12 repetitions
- Continue bike, stepper, cross trainer progression.
- Continue straight line running sprints / ball work to 75% straight runs.
- Continue progression of single plane power exercises – squats, calf raises, clean and jerk.
- Initiate multi-plane power exercises with weight and pulley resistance – trunk twists, twist push, pull backs.
- Progress functional running patterns:
Functional Running Pattern Exercises
Exercise 4
Variable pace running with gradual turns and various starting positions. The player starts at one end of the course makes a straight 30m run to a 20m diameter semi-circle, around which he gently turns before completing another straight 30m run back to the finish. The pace of the run is dictated by the physiotherapist and is either three quarter or full pace. The starting position should be different for each run (standing, lying on back, lying on front, sprint start position, squatting, right side lying, left side lying, jumping, hopping, facing backwards).
The player should complete 20 runs.
Exercise 5
Two 5m diameter circles are placed 30m apart. Travelling at full pace, the player makes a run with a football at his feet, goes round the far circle and then back to the finish.
This should be repeated 20 times.
Exercise 6
As Exercise 5, but single cones are used instead of 5m diameter circles.
Exercise 7
Six cones are placed 5m apart in a straight line. The player completes a shuttle run, at full pace, turning alternately to the left and right.
This should be repeated 10 times.
Post-op: Weeks 4 – 6
- Continue core strength exercises to 4 x 12 repetitions as a preventative strategy.
- Continue bike, stepper, cross trainer progression.
- Continue straight line running sprints/ball work to 100% straight runs.
- Progress to full functional training.
Gilmore’s Groin Prevention
Core strength and core stability exercises can improve muscle function across the trunk and pelvis. Core strength exercises on a mat using a swiss ball and resistance bands are ideal, because the improved muscular strength and stability can help to counteract the large forces that are applied to the lower abdomen and pelvis. This can reduce the risk of developing Gilmore’s Groin.


