What is Hip Arthritis?
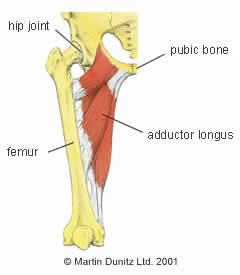
Hip arthritis (osteoarthritis) is a common cause of hip pain and hip stiffness that usually manifests itself in middle age. The term osteoarthritis is somewhat misleading, because its literal meaning is ‘joint inflammation’. Although there is a component of joint inflammation with this condition, the primary pathological process is progressive hip joint degeneration. In order to fully understand arthritis of the hip, it is probably helpful to review the anatomy of the hip joint.
The hip is a ‘synovial ball and socket joint’. This means that the ball of the femur and the socket of the pelvis that make up the hip joint are enclosed by a synovial capsule which contains synovial fluid. Synovial fluid lubricates the joint and provides nutrients to the tissues of the joint.
The joint surfaces of the ball and the socket are covered by hyaline cartilage, which provides friction free movement. There is a circular structure around the rim of the socket, called the acetabular labrum. The acetabular labrum is a shock absorber that is made of fibrocartilage. Damage to the labrum during sports can predispose someone to later arthritis of the hip. Both the ball (femur) and socket (pelvis) can be affected by arthritis.
Damage to the hyaline cartilage joint surfaces can be as a result of sporting trauma, but is more commonly due to repetitive stresses over a long period of time. Because the hip is an essential joint in weight-bearing, this is usually associated with habitual overuse of a joint for sporting but also occupational purposes, such as prolonged standing and walking. In most individuals, the signs and symptoms do not appear until middle age, but the disease process starts much earlier and the arthritis process can be accelerated following trauma to the hip joint.
The hyaline cartilage is normally ultra smooth to allow friction free movement, but early damage to the superficial layers produces a frayed appearance. In time, with more stress, this frayed surface evolves into cracks or ‘fissures’ in the articular cartilage, which can leave the underlying bone exposed to the point that there is bone on bone contact.
With continued wear the underlying bone takes on a polished appearance and eventually micro-fractures appear. The body’s natural reaction is to attempt to heal the micro-fractures by laying down more bone. This leads to a thickening of the underlying layer of bone, which can be seen on x-ray. Another common feature on x-ray is the formation of bone cysts in the layer of bone beneath the joint surface, together with a flattening of the joint surfaces as the body attempts to spread the surface area over which forces are transmitted.
As well as changes in the Hyaline cartilage and underlying bone, osteoarthritis produces soft tissue changes. As the joint becomes deformed by bony changes the ligaments which support the joint become stretched. There is also thickening and distension of the capsule that surrounds the joint and both of these features get progressively worse and can restrict movement at the joint.
Signs & Symptoms of Hip Arthritis
Hip pain is the most universal symptom of hip arthritis. This hip pain can be felt around the groin, but may also radiate down the thigh or up to the back. As the arthritis worsens and muscle wasting occurs there is often a pronounced limp. Weakness of the gluteal muscles means that the affected hip ‘drops’ during each walking step. This is known as a trendelenburg gait. The diagnosis of hip arthritis is confirmed with an x-ray which is characterised by a loss of joint space between the two bones.
Although osteoarthritis is a progressive disease, the signs and symptoms of the condition rarely get worse in a linear fashion. Often people in their thirties or forties will ‘overdo it’ one weekend, either in sport or in the garden, and they will experience a flare up from the degenerate joint. This flare up may last for 48 hours and usually consists of stiffness (particularly in the morning), pain and swelling of the affected joint.
Flare ups will settle with rest and the use of NSAIDs prescribed by a doctor. Ice therapy can also be helpful to relieve pain and reduce inflammation within the tissue. Ice packs can be applied for periods of twenty minutes every couple of hours (never apply ice directly to the skin as it can cause an ice burn).
A substantial time period may pass before there is another flare up, but each flare up will get progressively more intense. Also as time goes by and more stress is put on the affected joint, the time interval between flare ups will decrease to the point where, eventually, the person will have pain even at rest.
As the disease progresses the symptoms that start off being triggered by over activity, become triggered by immobility. Whereas, in the early stages, rest is essential during a flare up period, disuse in the later stages will exacerbate the problem. Evidence now suggests that gentle movement and exercise is beneficial for symptoms of osteoarthritis. This is because the dynamic stability provided by the muscles surrounding the joint is lost if there is muscle wasting due to inactivity. This puts even more strain on the ligaments and ultimately the joint surfaces themselves – producing more pain. In the later stages, if there is pain at rest and during the night, as well as problems with mobility, then joint replacement surgery is appropriate.
Treatment of Hip Arthritis
What you can do
- Consult a sports injury expert
- Use a buoyancy belt for mobilisation exercises in a swimming pool
- Use resistance bands for muscle strengthening exercises
- Wear compression shorts for reassurance following surgery
Patient education is one of the most effective treatment strategies. By understanding the nature of osteoarthritis the patient can make adjustments to their lifestyle that will make the problem more manageable. In summary, the patient must understand that too much activity or too little activity will make the problem worse. Maintaining a manageable level of low impact exercise such as walking is now thought to be extremely beneficial, even when osteoarthritis affects weight-bearing joints such as the hip. Each individual is different but, over time and through experience, each person will learn the optimum level of activity for their affected joint.
During the early phase, flare ups are best treated symptomatically. NSAIDs prescribed by a doctor are effective in relieving pain. Anti inflammatory gel can also help and doesn’t have the side effects associated with anti inflammatory tablets. An ice pack may be used to relieve a hot painful hip joint. Ice packs can be applied for periods of twenty minutes every couple of hours (never apply ice directly to the skin as it can cause an ice burn).
Many people find that wearing compression shorts can help provide support and reassurance. As Arthritis of the Hip tends to be more painful during cold winter months, compression garments and base layers are often helpful as it provides soothing warmth to the joint.
Once arthritis of the hip has been formally diagnosed a more long term preventative strategy can be undertaken. This is aimed at reducing pain and stiffness and maintaining range of movement in the affected joint. A sensible approach can prevent excessive degeneration which may eventually lead to disability.
Each individual case is different and a full assessment by a chartered physiotherapist will identify factors that may exacerbate the problem. Once identified, the physiotherapist will formulate a strategy to address these problems and an exercise regime can be developed. It may be that a work task is putting excessive repetitive stress on the affected joint. It may be possible to modify the task so it can be done in a different position, or specially adapted equipment can be used to reduce the repetitive loads. The main problem may be due to posture or a mal-alignment of the body.
Where the hip joint is affected maintenance of full range of motion is encouraged to reduce stiffness and loss of movement. Hip movement can be lost if the person doesn’t use the full range of motion because of pain and a characteristic, sequential loss of movement occurs. A physiotherapist can use manual techniques to help maintain the range of movement.
Pain in the hip joint can lead to an inhibition of the gluteal muscles. This leads to a vicious circle of further joint instability and more pain, leading to more inhibition and muscle weakness. Exercises using resistance bands to maintain gluteal muscle strength are encouraged to provide support for the affected joint. This strengthening should be done under the supervision of a physiotherapist.
If the hip joint is affected then weight bearing activities can make the problem worse. Running on a hard surface increases the stress on the joints and is not helpful for a person with osteoarthritis, even with shock absorbing insoles.
Swimming, because of its non weight bearing nature, is much more beneficial for the person with osteoarthritis of the hip. During this time hip function can be enhanced by performing non weight bearing exercises in the pool. A buoyancy belt allows an early return to swimming pool exercises for people with arthritis of the hip. It clips around the waist and allows the user to exercise without putting weight through their injury.
Where hip pain due to hip arthritis significantly reduces quality of life, then hip replacement surgery should be considered. It is an extremely successful operation in the vast majority of cases, leading to a dramatic restoration of function. However, despite many technical advances in replacement hip joint design, the new joint has a limited life span. Surgeons therefore prefer not to undertake hip replacement surgery in younger patients who have hip arthritis. Alternative surgical techniques such as hip joint re-surfacing may be more appropriate in younger patients. Hip re-surfacing involves placing a metal cup in the hip socket and a metal cap over the ball of the joint.
Prevention of Hip Arthritis
In addition to avoiding weight bearing and impact exercises, prolonged sitting should be avoided, as should sitting in one position for a period of time. Frequent breaks should be taken to stretch and take the hip joint through it’s full range of motion, as the articular cartilage draws most of it’s nourishment from the synovial fluid within the joint, and this has the effect of providing nutrients to the joint surfaces. Prolonged sitting will also prevent the gluteal muscles from working efficiently so regular breaks will help restore their function isn’t compromised.


